Rheumatoid Arthritis
Improvement of Oral Hygiene in Patients with Rheumatoid Arthritis
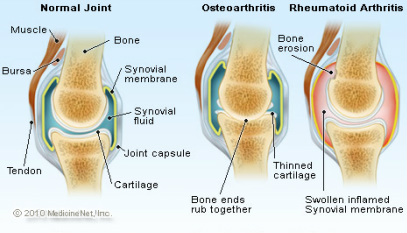
The journal article I chose to discuss is written by H Risheim, V Kjarheim, and P Arneberg. This article discusses rheumatoid arthritis and its affect on oral hygiene in patients with the condition. The condition usually affects salivary gland function which results in a reduction of saliva that makes these patients more susceptible for caries involvement. This factor alone makes good oral hygiene care imperative. These patients could benefit by using an electric toothbrush which requires less dexterity and strength when compared to a manual toothbrush. The authors begin by stating that patients who suffer from RA have swelling and tenderness of joints that can impair manual dexterity. RA is more commonly seen two-three times in women than men and occurrence is usually during the fourth or fifth decade of life. The study showed that three of four patients who have RA reported constant problems while performing oral hygiene tasks.
The clinical trial was designed to test plaque reducing effects of three different oral hygiene regimens seen in RA patients. The first group was instructed to use traditional manual toothbushing, the second group was instructed to use an electric toothbrush, and the third was instructed to use manual toothbrusing using fluoride/chlorhexideine gel as a toothpaste. A 2-week control period was implemented where patients were instructed to continue brushing their teeth as they usually would. Then three consecutive 2-week experimental periods occurred by the same examiner in a randomized sequence. At the beginning of the experiment, each person had their teeth cleaned professionally using a rubber cup and pumice. All patient compliance was supervised by the instructor. The patients in the manual toothbrushing group was given a multitufted soft brush and instructed to use a horizontal brushing technique with emphasis on short movements. The patients in the electric toothbrushing group was given a soft brush head and instructed to used a combination of vertical and horizontal brush movements. The manual toothbrushing with fluoride/chlorhexidine gel group was instructed to us gel containing .2% sodium fluoride, 1% chlorhexidine digluconate, 3% carboxymethyl-cellulose and flavor with no abrasives.
At the end of each control period, the buccal and lingual surfaces of all teeth were disclosed in solution and examined. The result were recorded from 1-4. Meaning a score of 1 meant it was covering less than 1/3 of the tooth without a continuous rim of plaque adjacent to the gingival margin, a score of 2 meant plaque covered less than 1/3 of the tooth surface forming a continual rim of plaque adjacent to the gingival margin, a score of 3 meant plaque deposits covered more than 1/3 of the tooth surface adjacent to the gingival margin and less than 2/3 of the surface, and finally a score of 4 meant plaque was covering more than 2/3 of the tooth surface. Mobility of the patients shoulders, elbows, wrists, and finger joints was also evaluated by the examiner and listed as normal, moderately, or severely impaired.
The results of the study gave no changes in the plaque status, although there was considerable reduction observed in the three experimental regimens. The largest improvement was found in the group that using manual brushing with chlorhexidine/fluoride gel. The group using electric toothbrushing showed reduction of plaque scores more than manual brushing did with regular toothpaste. The joints of the patients fingers and wrists were affected by RA frequently, but there was no clear relationship between the findings and oral hygiene or improvement of the oral cavity. Brown discoloration was noted on the group using chlorhexiden/fluoride. Three of the patients were displeased with this discoloration and one had even stopped using the gel after only 2 days. One patient developed signs of geographic tongue and another reported recurrent intraoral HSV-infection during the period of use. At the final conclusion of the study, 11 of 14 patients wanted to switch from manual toothbrushing to an electric toothbrush.
Concluding the article, the authors assert that toothbrushing is the most widely accepted remedy for daily removal of plaque and that though interdental plaque control is less widespread, it is important for oral health. Interdental care can pose a problem for patients who have RA, but it was not evaluated in this study. The difference in plaque removal between manual toothbrushing and electric brushing was small and the practicality of using chlorhexidine/fluoride gel is limited due to its poor taste and discoloration.
I chose to discuss Rheumatoid Arthritis, because I honestly had no idea what it was. I knew it was associated with bone and joints, but I was not sure of anything else pertaining to RA. I thought it would be an interesting topic to research and be familiar with since it would heavily affect my future patients oral hygiene care.
Reference
Risheim, H., Kjærheim, V., & Arneberg, P. (1992). Improvement of oral hygiene in patients with rheumatoid arthritis. Scandinavian Journal Of Dental Research, 100(3), 172-175.
Additional Information
Photo from Google Image
Article from Ebscohost
The clinical trial was designed to test plaque reducing effects of three different oral hygiene regimens seen in RA patients. The first group was instructed to use traditional manual toothbushing, the second group was instructed to use an electric toothbrush, and the third was instructed to use manual toothbrusing using fluoride/chlorhexideine gel as a toothpaste. A 2-week control period was implemented where patients were instructed to continue brushing their teeth as they usually would. Then three consecutive 2-week experimental periods occurred by the same examiner in a randomized sequence. At the beginning of the experiment, each person had their teeth cleaned professionally using a rubber cup and pumice. All patient compliance was supervised by the instructor. The patients in the manual toothbrushing group was given a multitufted soft brush and instructed to use a horizontal brushing technique with emphasis on short movements. The patients in the electric toothbrushing group was given a soft brush head and instructed to used a combination of vertical and horizontal brush movements. The manual toothbrushing with fluoride/chlorhexidine gel group was instructed to us gel containing .2% sodium fluoride, 1% chlorhexidine digluconate, 3% carboxymethyl-cellulose and flavor with no abrasives.
At the end of each control period, the buccal and lingual surfaces of all teeth were disclosed in solution and examined. The result were recorded from 1-4. Meaning a score of 1 meant it was covering less than 1/3 of the tooth without a continuous rim of plaque adjacent to the gingival margin, a score of 2 meant plaque covered less than 1/3 of the tooth surface forming a continual rim of plaque adjacent to the gingival margin, a score of 3 meant plaque deposits covered more than 1/3 of the tooth surface adjacent to the gingival margin and less than 2/3 of the surface, and finally a score of 4 meant plaque was covering more than 2/3 of the tooth surface. Mobility of the patients shoulders, elbows, wrists, and finger joints was also evaluated by the examiner and listed as normal, moderately, or severely impaired.
The results of the study gave no changes in the plaque status, although there was considerable reduction observed in the three experimental regimens. The largest improvement was found in the group that using manual brushing with chlorhexidine/fluoride gel. The group using electric toothbrushing showed reduction of plaque scores more than manual brushing did with regular toothpaste. The joints of the patients fingers and wrists were affected by RA frequently, but there was no clear relationship between the findings and oral hygiene or improvement of the oral cavity. Brown discoloration was noted on the group using chlorhexiden/fluoride. Three of the patients were displeased with this discoloration and one had even stopped using the gel after only 2 days. One patient developed signs of geographic tongue and another reported recurrent intraoral HSV-infection during the period of use. At the final conclusion of the study, 11 of 14 patients wanted to switch from manual toothbrushing to an electric toothbrush.
Concluding the article, the authors assert that toothbrushing is the most widely accepted remedy for daily removal of plaque and that though interdental plaque control is less widespread, it is important for oral health. Interdental care can pose a problem for patients who have RA, but it was not evaluated in this study. The difference in plaque removal between manual toothbrushing and electric brushing was small and the practicality of using chlorhexidine/fluoride gel is limited due to its poor taste and discoloration.
I chose to discuss Rheumatoid Arthritis, because I honestly had no idea what it was. I knew it was associated with bone and joints, but I was not sure of anything else pertaining to RA. I thought it would be an interesting topic to research and be familiar with since it would heavily affect my future patients oral hygiene care.
Reference
Risheim, H., Kjærheim, V., & Arneberg, P. (1992). Improvement of oral hygiene in patients with rheumatoid arthritis. Scandinavian Journal Of Dental Research, 100(3), 172-175.
Additional Information
Photo from Google Image
Article from Ebscohost
