Oral Health During Pregnancy
Description
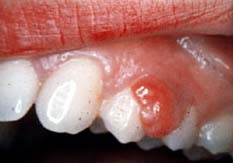
Increases in hormone levels have an effect on the periodontium especially when there is preexisting plaque-induced gingival inflammation present. An increase of gingival inflammation is seen in pregnant women due to this increase of hormone levels. Inflammation that is initiated by plaque-biofilm is exacerbated by hormonal changes that occur in the second and third trimesters. With pregnancy gingivitis, we see an increase in bleeding on probing, and crevicular fluid present in the sulcular tissues. Pregnant women produce large amounts of estradiol, estriol, and progesterone which in the eight month are at their peak, resulting in the highest incidence of inflammation. These high hormone levels can also affect host response to plaque-biofilm by suppressing the immune response and altering PMN chemotaxis and phagocytosis. In some cases, the interdental papilla can have a strong reaction to bacterial plaque-biofilm that causes large localized growths to occur. This is termed a pregnancy-associated pyogenic granuloma or pregnancy tumor as shown in the above picture.
Diagnostic Factors
Pregnancy gingivitis and pregnancy-associated pyogenic granulomas are diagnosed by a clinical appearance consisting of deep red or purplish gums that will bleed easily that has a rapid onset during the second or third trimester of their pregnancy.
Etiology
It is caused by an increase in hormones such as estradiol, estriol, and progesterone along with local irritants and bacteria.
Pathogens Associated
Increases in the periodontal pathogen, P. intermedia is seen in pregnant women compared with non-pregnant women.
AAP Classificiation
I-A dental plaque-induced gingival disease with modifying factors
Prevalence
5% of women will develop pregnancy gingivitis during their pregnancy.
Patient Education
Pregnant patients should be:
>Educated on the effects of pregnancy on their gingival tissues
>We as dental hygienist need to express the importance
of thorough at home self-care for removal and control of plaque-biofilm
>We also need to ensure that the patient understands that professional care should be implemented during this time as well
Treatment Recommendations or Corrective Procedures
-Each pregnant patient should:
>Be evaluated for their dental hygiene habits and oral problems (ex. caries, gingivitis)
>Access to fluoridated water
>Access to professional dental care
>Directed to perform routine brushing and flossing
>Instructed to avoid excessive amounts of sugary snacks and drinks
-Pregnant patients should also be aware of factors that can reduce the caries risk for their children:
>Use of Xylitol and chlorhexidine to lower maternal oral bacterial load that could be transferred to the infant during pregnancy as well as after pregnancy or during breast feeding
-Treatment should be performed only if necessary and should only be carried out during the second trimester when organogenesis is completed
-If treatment is necessary the appointments should be brief and the patient should be propped on her left side and repositioned often
Maintenance Recommendations
The patient should have excellent home care regimens in place during pregnancy and also post-pregnancy. The patient should continue with routine dental cleanings and seek dental treatment only as needed during pregnancy.
References
Silk, H., Douglass, A., Douglass, J., & Silk, L. (2008). Oral health during pregnancy. American Family Physician, 77(8), 1139-1144.
Ibsen, O. Andersen Phelan, J. Oral Pathology for the Dental Hygienist, Fifth Edition.
Nield-Gehrig, J., Willmann, D., (2011). Foundations of Periodontics for the Dental Hygienist, Third Edition
Additional Information
Photos from Google Image
Article form Ebscohost
Increases in hormone levels have an effect on the periodontium especially when there is preexisting plaque-induced gingival inflammation present. An increase of gingival inflammation is seen in pregnant women due to this increase of hormone levels. Inflammation that is initiated by plaque-biofilm is exacerbated by hormonal changes that occur in the second and third trimesters. With pregnancy gingivitis, we see an increase in bleeding on probing, and crevicular fluid present in the sulcular tissues. Pregnant women produce large amounts of estradiol, estriol, and progesterone which in the eight month are at their peak, resulting in the highest incidence of inflammation. These high hormone levels can also affect host response to plaque-biofilm by suppressing the immune response and altering PMN chemotaxis and phagocytosis. In some cases, the interdental papilla can have a strong reaction to bacterial plaque-biofilm that causes large localized growths to occur. This is termed a pregnancy-associated pyogenic granuloma or pregnancy tumor as shown in the above picture.
Diagnostic Factors
Pregnancy gingivitis and pregnancy-associated pyogenic granulomas are diagnosed by a clinical appearance consisting of deep red or purplish gums that will bleed easily that has a rapid onset during the second or third trimester of their pregnancy.
Etiology
It is caused by an increase in hormones such as estradiol, estriol, and progesterone along with local irritants and bacteria.
Pathogens Associated
Increases in the periodontal pathogen, P. intermedia is seen in pregnant women compared with non-pregnant women.
AAP Classificiation
I-A dental plaque-induced gingival disease with modifying factors
Prevalence
5% of women will develop pregnancy gingivitis during their pregnancy.
Patient Education
Pregnant patients should be:
>Educated on the effects of pregnancy on their gingival tissues
>We as dental hygienist need to express the importance
of thorough at home self-care for removal and control of plaque-biofilm
>We also need to ensure that the patient understands that professional care should be implemented during this time as well
Treatment Recommendations or Corrective Procedures
-Each pregnant patient should:
>Be evaluated for their dental hygiene habits and oral problems (ex. caries, gingivitis)
>Access to fluoridated water
>Access to professional dental care
>Directed to perform routine brushing and flossing
>Instructed to avoid excessive amounts of sugary snacks and drinks
-Pregnant patients should also be aware of factors that can reduce the caries risk for their children:
>Use of Xylitol and chlorhexidine to lower maternal oral bacterial load that could be transferred to the infant during pregnancy as well as after pregnancy or during breast feeding
-Treatment should be performed only if necessary and should only be carried out during the second trimester when organogenesis is completed
-If treatment is necessary the appointments should be brief and the patient should be propped on her left side and repositioned often
Maintenance Recommendations
The patient should have excellent home care regimens in place during pregnancy and also post-pregnancy. The patient should continue with routine dental cleanings and seek dental treatment only as needed during pregnancy.
References
Silk, H., Douglass, A., Douglass, J., & Silk, L. (2008). Oral health during pregnancy. American Family Physician, 77(8), 1139-1144.
Ibsen, O. Andersen Phelan, J. Oral Pathology for the Dental Hygienist, Fifth Edition.
Nield-Gehrig, J., Willmann, D., (2011). Foundations of Periodontics for the Dental Hygienist, Third Edition
Additional Information
Photos from Google Image
Article form Ebscohost
