Bisphosphonate Therapy and Dental Hygiene
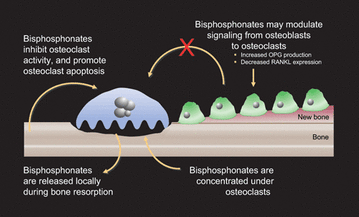
Osteoporosis is a decrease in bone mass that causes bone to become more prone to fracture. It is caused by an increase in osteoclast activity with a decrease in osteoblast activity. Osteoclasts are responsible for bone resorption and osteoblasts are responsible for bone formation. During younger years of life osteoblast activity is greater than osteoclast activity and as we age, osteoblast activity is slowly depleted. There are two types of Osteoprosis: Primary Osteoporosis, and Secondary Osteoporosis.
Primary Osteoporosis is broken down into two types. Type I occurs in women before, during, or after menopause as a result of lowered estrogen levels. Type II occurs around age 75 as a result of normal effects of aging. Secondary Osteoporosis results from intake of certain medications or medical conditions. Treatment options for this condition include intake of calcium and vitamin D, exercise, hormone replacement therapy, Calcitonin, Raloxifine, sodium fluoride, and bisphosphonates. As dental hygienists we are concerned with bisphosphonate therapy.
Bisphosphonates are commonly prescribed for osteopenia or osteoporosis. This type of therapy inhibits osteoclasts and increase osteoblast effectiveness. However, they are not metabolized or excreted resulting in a very long half-life of about 10 years and have been seen to result in osteonecrosis of the jaw. The journal article I choose is written by DeeAnne Aschcroft, RDH, BS, MPH and discusses Ramifications of bisphosphonate therapy and dental hygiene.
Ashcroft asserts that bisphosphonates serve to help slow down and prevent bone loss that is associated with osteoporosis, but can also potentially lead to necrosis of the jaw. She also says that recent studies have shown that bisphosphonates inhibit angiogenesis which can lead to avascular bone conditions. She continues to state that clinical drug testing with this therapy appeared to be safe and very effective and it wasn't until after marketing that bisphosphonate-induced ONJ began to arise. The risk for developing ONJ increases with the duration the drug is taken.
Oral manifestations seen clinically include small or large, painful or asymptomatic, localized disfigured lesions. The presence of this condition is diagnosed when there is exposed bone in the oral area whether it be spontaneous or induced by treatment that does not heal with in 6 weeks. She adds that treatment for the condition is challenging, because normal treatment procedures consisting of antibiotics, anti-infectives, debridement and flap coverage do not consistently respond and have sometimes led to a greater surface involvement.
Ashcroft stated that in her years as a hygienist, she has yet to come across a patient who has been properly informed by their physician about the possible risk for taking this drug therapy, thus making it very important to educate patients about bisphosphonates and their condition. It is recommended that a patient have any dental treatment taken care of two months prior to beginning therapy. Treatment would include, periodontal treatment and extractions of non-vital teeth to avoid disruption of bone once therapy has started. She also stated that it is important to continue dental treatment that doesn't necessarily need to be altered unless treatment will effect the bone and most importantly to make sure the patients understand the importance of maintaining good at home oral hygiene so that problems do not arise during treatment.
This article is relevant to dental hygiene, because as hygienist, it is our job to encourage patients at risk for ONJ to develop and maintain good oral home care that will help minimize the need for dental treatment while on this type of drug therapy. It is also relevant, because we tend to be the most familiar with our patients medications and health histories. Our Doctors rely on us to relay important updates at every visit so that everything runs smoothly in the practice.
I chose to this condition to discuss, because I was not very familiar with osteoporosis. I have heard commercials about it, heard about the medications that help to slow the process, but I never fully understood what the condition was. After learning about osteoporosis, I thought it very interesting that bisphosphonate drugs are meant to help the condition, but yet in the long run, they actually cause destruction.
DeeAnne Ashcroft, RDH, BS, MPH, February 1, 2007. The Dental Hygiene Ramifications of Bisphosphonate Therapy
Additional Information
Picture from google
Video animation from YouTube
Primary Osteoporosis is broken down into two types. Type I occurs in women before, during, or after menopause as a result of lowered estrogen levels. Type II occurs around age 75 as a result of normal effects of aging. Secondary Osteoporosis results from intake of certain medications or medical conditions. Treatment options for this condition include intake of calcium and vitamin D, exercise, hormone replacement therapy, Calcitonin, Raloxifine, sodium fluoride, and bisphosphonates. As dental hygienists we are concerned with bisphosphonate therapy.
Bisphosphonates are commonly prescribed for osteopenia or osteoporosis. This type of therapy inhibits osteoclasts and increase osteoblast effectiveness. However, they are not metabolized or excreted resulting in a very long half-life of about 10 years and have been seen to result in osteonecrosis of the jaw. The journal article I choose is written by DeeAnne Aschcroft, RDH, BS, MPH and discusses Ramifications of bisphosphonate therapy and dental hygiene.
Ashcroft asserts that bisphosphonates serve to help slow down and prevent bone loss that is associated with osteoporosis, but can also potentially lead to necrosis of the jaw. She also says that recent studies have shown that bisphosphonates inhibit angiogenesis which can lead to avascular bone conditions. She continues to state that clinical drug testing with this therapy appeared to be safe and very effective and it wasn't until after marketing that bisphosphonate-induced ONJ began to arise. The risk for developing ONJ increases with the duration the drug is taken.
Oral manifestations seen clinically include small or large, painful or asymptomatic, localized disfigured lesions. The presence of this condition is diagnosed when there is exposed bone in the oral area whether it be spontaneous or induced by treatment that does not heal with in 6 weeks. She adds that treatment for the condition is challenging, because normal treatment procedures consisting of antibiotics, anti-infectives, debridement and flap coverage do not consistently respond and have sometimes led to a greater surface involvement.
Ashcroft stated that in her years as a hygienist, she has yet to come across a patient who has been properly informed by their physician about the possible risk for taking this drug therapy, thus making it very important to educate patients about bisphosphonates and their condition. It is recommended that a patient have any dental treatment taken care of two months prior to beginning therapy. Treatment would include, periodontal treatment and extractions of non-vital teeth to avoid disruption of bone once therapy has started. She also stated that it is important to continue dental treatment that doesn't necessarily need to be altered unless treatment will effect the bone and most importantly to make sure the patients understand the importance of maintaining good at home oral hygiene so that problems do not arise during treatment.
This article is relevant to dental hygiene, because as hygienist, it is our job to encourage patients at risk for ONJ to develop and maintain good oral home care that will help minimize the need for dental treatment while on this type of drug therapy. It is also relevant, because we tend to be the most familiar with our patients medications and health histories. Our Doctors rely on us to relay important updates at every visit so that everything runs smoothly in the practice.
I chose to this condition to discuss, because I was not very familiar with osteoporosis. I have heard commercials about it, heard about the medications that help to slow the process, but I never fully understood what the condition was. After learning about osteoporosis, I thought it very interesting that bisphosphonate drugs are meant to help the condition, but yet in the long run, they actually cause destruction.
DeeAnne Ashcroft, RDH, BS, MPH, February 1, 2007. The Dental Hygiene Ramifications of Bisphosphonate Therapy
Additional Information
Picture from google
Video animation from YouTube
